Scars
Almost everyone gets scars on their bodies, from the smallest leftover scrape to the much larger wounds from a car accident or surgery. What you may not know is that there are different kinds of scars, and the type of scar you have may determine if you are able to have scars removed successfully at some time in the future. If you decide that you’d like to try to have a scar revised or removed, it’s helpful to know what type of scar you have before you visit your New York dermatologist. At your appointment, a good dermatologist can determine whether you’d be a good candidate for a procedure to improve the appearance of your scars. While there are other factors when trying to remove scars, the first is identifying the type of scar you have.
Surface Irregularities or Discolorations
These are scars that don’t cause you pain or impair your function. Surface irregularities or discolorations are flat and pale. They form after an injury as a result of your body’s natural healing process. They may start out as red and raised, but over a period of time, they become flattered and blend better into your skin. If the edges of your scar have come together neatly, you should have little remaining other than a thin pale line after about two years. It may never disappear completely, but it won’t be easily visible. If you have darker skin, the scar tissue may fade and leave a white or brown mark. Most acne scars and scars from minor wounds fall into this category.
Hypertrophic Scars
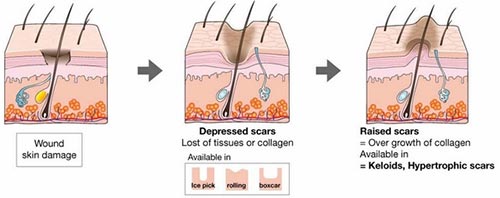
A hypertrophic scar is made up of thick clusters of scar tissue on the wound site. It’s the result of an imbalance of collagen in your skin during the healing process. The build-up eventually causes the scar tissue to grow thicker and less flexible than your surrounding skin. This scar is raised and red, and it can be uncomfortable. Over time, it becomes not only thicker and wider but also darker or lighter than your skin color. It may restrict your movement because the scar is not as flexible as the surrounding skin. While it doesn’t extend beyond the boundaries of your original wound, the skin continues to get thicker, month after month, for up to five years.
Keloids
A keloid scar is bigger than a hypertrophic scar. But like a hypertrophic scar, a keloid is also caused by excess collagen produced during the healing process. This can cause an overgrowth of tissue, continuing to grow even after the original wound has healed. Keloid scars can be painful or itchy, and they can pucker your skin. Unlike hypertrophic scars, they can extend over the edges of the original incision or wound. You can develop a keloid anywhere on your body, but they’re most commonly found where you have little fatty tissue, such as on your shoulders, chest, neck, face, or ears. There are other characteristics of Keloid scars as well, such as:
- They can be much larger than the original wound.
- They’re often hairless and shiny.
- They can have a hard, rubbery, or lumpy texture.
- They’re often raised above the skin.
- They can cause a burning sensation or tenderness in the affected area.
- They’re red or purple when newly formed, but they become paler over time.
Contractures
Contractures are scars that restrict your movement. These scars can be caused by the tissues underlying your wound that pull together during healing. A contracture can form when you lose a lot of tissue, such as from a large burned area. You can also get a contracture over a joint, which restricts its movement. Contractures can affect your neck, elbows, knees, or fingers. When the tissue underlying your skin is lost, for whatever reason, the skin above it shrinks as it heals. This healing action causes your skin to lose elasticity, which in turn restricts your movement in the affected area. While it’s most noticeable when it happens over a joint, it can impact your movement and flexibility no matter where it occurs.
Pitted or Sunken Scars
Also called ice-pick scars or atrophic scars, these scars have a pitted or sunken appearance. Like contractures, it’s the loss of underlying collagen that forms these scars. Unlike contractures, these scars aren’t raised. You may have pitted or sunken scarring due to severe acne or chickenpox. You can have this kind of scar from burns that may have resulted in the loss of underlying tissues. Other causes include certain surgeries and accidents.
Stretch Marks
Stretch marks first appear on your skin as flattened pink areas that then develop the characteristic purple streaks or lines on your skin. Their color can vary from pink to dark brown, depending on your skin color. They can occur anywhere that your skin has been stretched, usually in areas where fat is stored. Both men and women can develop stretch marks. Some teenage boys can develop horizontal stretch marks over their spines, similar to rungs on a ladder. Other common areas to see stretch marks include:
- Stomach
- Upper arms
- Buttocks
- Breasts
- Thighs
- Shoulders, mainly on bodybuilders
Stretch marks develop after rapid changes in your body or due to underlying health conditions such as:
- Your skin stretches to accommodate the growing fetus.
- You may grow quickly during puberty, causing your skin to stretch.
- Rapid weight gain. Your skin stretches to fit over your larger body mass.
- Family history of stretch marks. Your family may be prone to developing stretch marks.
- Cushing’s syndrome. Your body produces too much cortisol, which is thought to cause stretch marks.
- Marfan syndrome. A faulty gene causes weakness in your body’s connective tissues and skin, making them less elastic and able to stretch. This leads to the development of stretch marks, most commonly on your shoulders, hips, and lower back.
Overuse of corticosteroids can also lead to the development of stretch marks. Creams or lotions containing steroids used for other skin conditions can reduce the amount of collagen in your skin. Collagen is the protein that helps keep your skin flexible. When it’s reduced, you’re more likely to develop stretch marks. Be sure to use any topical medication containing steroids as directed by your doctor.
Important Reminder: This information is only intended to provide guidance, not definitive medical advice. Please consult dermatologist NYC about your specific condition. Only a trained, experienced board certified dermatology doctor or pediatric dermatologist could determine an accurate diagnosis and proper treatment.
Locations: Manhattan Dermatology (Upper East Side) 983 Park Ave, Ste 1D1, NY 10028(212) 427-8750 Manhattan Dermatology (Midtown) 56 W 45th St, Ste 819, NY 10036
(212) 889-2402 Manhattan Dermatology (Union Square) 55 W 17th St, Ste 103, NY 10011
(212) 378-9984

