Keratosis Pilaris
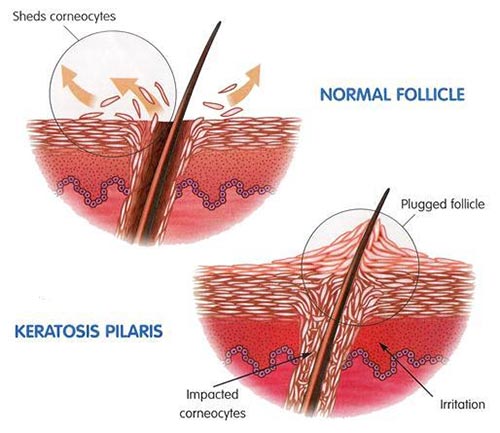
If you’ve contracted a skin condition that seems like acne or small pimples but doesn’t respond to the usual treatments, you may very well have keratosis pilaris. A visit to the dermatology office can “clear things up” about the nature of your skin condition and how to treat it. Keratosis pilaris is rough bumps on your skin that some say look like the skin of a plucked chicken. If you do have keratosis pilaris, don’t be alarmed. It’s a very common skin condition made up of clumps of dead skin cells on the surface of your skin. These clumps or plugs usually appear on your upper arms and the front of your thighs. Children may develop this skin condition on their faces and cheeks.
Symptoms of Keratosis Pilaris
Your arms, thighs, and other areas where you develop keratosis pilaris may become dry and itchy. If your skin is dry, the effects of keratosis are more noticeable. People who live in a dry climate find they only develop this skin condition in the winter when it’s drier. If you live in a warm, dry climate and swim throughout the year, you may experience this condition year-round. If you spend a lot of time in direct sunlight, you may have a solar keratosis variation.
This condition, also known as actinic keratosis, appears as scaly, rough patches on your face and head. Older people are more at risk of experiencing this skin condition, which is harmless. However, there is a small risk of becoming skin cancer, so you should visit your dermatologist to receive a full examination and any recommended treatment.
Treating Keratosis Pilaris
There is no known cure for keratosis pilaris. But don’t lose heart if you have it. In some cases, it goes away on its own. In others, its symptoms can be controlled and treated. Talk to your dermatologist about the treatments that may work best for you. Fortunately, there are many skincare recipes and treatment options available to you.
People get the condition for a variety of reasons. Plus, different people have different types of complexions. These and other factors prohibit a one-size-fits-all treatment. No therapy for keratosis pilaris is effective for everyone across the board. So you may have to try several treatments before you find some that work for you.
One general treatment to prevent dry skin is using a mild cleanser that doesn’t contain soap, such as Cetaphil or Dove. Exfoliation is also helpful for getting rid of the small plugs of keratin in the top layers of your skin. The best results are typically found by combining therapies.
You can see improvement by adhering to an ongoing skincare plan. Many people respond well to skincare programs designed to treat keratosis. Just remember that treatment has to be ongoing. If you don’t use the lotions or therapeutic creams as directed, the condition can return. In some cases, a complete clearing of keratosis isn’t possible even when diligently following the treatment plan.
Prescription Medication for Keratosis
Dermatology doctors may prescribe a topical steroid cream like Cloderm or Locoid Lipocream. These are typically prescribed for seven to 10 days, applied one to two times daily to inflamed or red areas. Once the swelling is reduced successfully, you can treat the remaining rough, dry bumps with a mixture of urea cream and salicylic acid. Another effective treatment for keratosis is the intermittent application of topical retinoids. These are stronger medicines that are applied weekly or biweekly. When your condition starts to clear, milder creams may be used as part of an ongoing regimen.
Co-Occurring Conditions
If you are experiencing hyperpigmentation, which is ongoing skin discoloration, you can treat it with a fading cream that contains hydroquinone (HQ), azelaic acid, and kojic acid. If your skin discoloration is more extreme, consult your dermatologist for specific treatments. You may need a stronger concentration of HQ — possibly six, eight, or 10 percent. Be aware that a higher concentration of HQ can cause irritation and possibly even ochronosis, during which your skin may turn a bluish-black color. Topical immunomodulators are also effective at treating keratosis. These include creams with the active ingredient tacrolimus or pimecrolimus, which go by Protopic and Elidel’s brand names. These treatments are typically used if you have severe inflammation or redness in the affected area.
Light Therapy for Keratosis
Dermatologists may also suggest a two-step combination of a light source and topical photosensitizer for temporary treatment of keratosis. Light sources such as sunlight, red light, blue light devices activate a chemical in the photosensitizer that temporarily treats keratosis. This type of photodynamic therapy can be useful for severe cases when you need relief quickly. Unfortunately, it doesn’t offer long-term treatment, but light therapy can be used in conjunction with other, more lasting treatments.
Surgical Care for Keratosis Pilaris
If creams and other treatments aren’t effective in treating your keratosis, your dermatologist may recommend surgical treatments, such as a minor surgery called gentle acne extraction. This surgery is performed with a diabetic lancet to cut the skin. Then instruments are used to remove the trapped coiled hairs or keratin plugs formed below the skin, causing your keratosis. Your dermatologist can perform several surgical procedures as well as more conventional treatments right in the office. These include:
- Dermabrasion;
- Microdermabrasion;
- Abrasion, which uses a synthetic diamond to exfoliate your skin and a vacuum to remove dead skin cells;
- Chemical peels;
- Photodynamic therapy;
- Laser treatments;
- Blue light therapy;
- Pulsed light instruments;
- Surgical extraction of trapped hairs or keratin plugs.
There are possible side effects related to surgery and the other treatments listed above for keratosis. The risks include skin tautness, redness, swelling, skin sensitivity, and slight bruising. All these side effects are temporary and relatively minor.
Preventing Keratosis Pilaris
Your dermatology specialist may provide you with in-home treatments to keep your keratosis from returning. Proceed with care and make sure you follow the dermatologist’s directions and maintain the prescribed therapy regimen. At-home therapies include:
- Retinol creams;
- Exfoliation pads such as Buf-Puff;
- Topical emollients;
- Gentle suction exfoliation, such as Vacubrasion;
- Glycolic acid peels with a strength of 10 to 20 percent.
You can prevent your keratosis from becoming worse and possibly prevent it entirely by taking measures to prevent dry skin. Some of these measures include frequently applying emollients and cleaning with mild soaps and cleansers that don’t contain soap.
Keratosis Pilaris FAQ
What Is Keratosis Pilaris?
Keratosis pilaris (KP) is commonly referred to as a harmless skin condition that leads to dry, rough patches and tiny bumps. They typically appear on the thighs, upper arms, cheeks, or buttocks. These bumps do not tend to itch or hurt. This skin disorder cannot be cured or prevented. However, it can be managed with moisturizers and prescription creams to improve the appearance of the skin. KP normally disappears by the age of 30.
What Are the Causes of Keratosis Pilaris?
This skin disorder is believed to result from the buildup of keratin, which is a hard protein that protects the skin from harmful infections and harmful substances. Keratin forms a scaly plug that blocks the opening of the hair follicle. Normally, many plugs form, causing patches of bumpy and rough skin. It is still to be discovered why keratin builds up. Although, it may occur because of genetic diseases or in association with other skin conditions. Keep in mind that dry skin has been shown to worsen keratosis pilaris symptoms.
How to Get Rid of Keratosis Pilaris?
Keratosis pilaris, also known as chicken skin, cannot be cured, but you can still manage its symptoms if you do not feel confident about your skin looks. This skin condition typically disappears by itself as a person ages. KP skin condition is generally treatment-resistant, but several methods can ease its symptoms. It is also possible to address this skin disorder in-home settings using a warm bath, exfoliation, coconut oil, and humidifiers. People who got exposed to KP should also avoid wearing tight clothes.
What Does Keratosis Pilaris Look Like?
Keratosis pilaris causes hard and small bumps that make a person’s skin feel like sandpaper. These bumps are normally light-colored, and they sometimes appear with redness and/or swelling. Furthermore, they can also show up on the face, but it is very uncommon.
Who Is Prone to Developing Keratosis Pilaris?
People with the following health conditions are at a higher risk of developing “chicken skin”: dry skin, ichthyosis, eczema, hay fever, melanoma, obesity, and Celtic ancestry. Chicken skin is more common in teenagers and children. However, you need to be aware that anyone can encounter a KP skin condition, and it typically clears up by the age of 30.
Important Reminder: This information is only intended to provide guidance, not definitive medical advice. Please consult a dermatologist about your specific condition. Only a trained, experienced board-certified dermatology doctor or pediatric dermatologist can determine an accurate diagnosis and proper treatment.
(212) 427-8750 Manhattan Dermatology (Midtown) 56 W 45th St, Ste 819, NY 10036
(212) 889-2402 Manhattan Dermatology (Union Square) 55 W 17th St, Ste 103, NY 10011
(212) 378-9984

